Fatty acids and triglycerides.
Note: This is an updated version of the blog post on fatty acids and triglycerides.
The following question was posted on Facebook:
I had thought that free fatty acids were triglycerides. But I am reading a study that measured both. Can someone enlighten me on free fatty acids? … please.
Start with the carboxylic acids all of which have the carboxyl (-COOH) functional group. Recall that fatty acids are long chain carboxylic acids. Review of structure below:
All dietary and body fats and oils are triglycerides (TG) or, more correctly, triacylglycerols (TAG), that is, esters of the alcohol glycerol with three fatty acids. (The term “acyl” (pr. A-sill) is the adjective form of acid).
Fats have a roughly E-shaped structure. The arms of the E are the fatty acids. The fatty acids provide the real fuel in fats. The three fatty acids are attached to the compound glycerol which is the vertical stroke of the E. The chemical bond that attaches the fatty acid to the glycerol is called an ester bond. You need to know the term ester because when the fatty acids are found alone, especially in blood, they are referred to either as free fatty acids (FFA) or, because they are no longer attached to the glycerol by the ester bonds, as non-esterified fatty acids (NEFA): FFA and NEFA are the same thing.
Metabolism: the fatty acid-TAG cycle.
The digestion of fat in the intestine involves the progressive removal of the fatty acids from the first and last position of the glycerol. The process is called lipolysis and the enzyme that catalyzes the reaction is called a lipase. What remains is called 2-monoacylglycerol, or 2-MAG (fatty acid still attached at the center carbon of glycerol) and 2-MAG and the free fatty acids from digestion are absorbed into the intestinal cells. Within these cells they are re-formed into TAG which is exported together with cholesterol and other components in particles called chylomicrons. Chylomicrons, in turn, represent one type of complex structure known as lipoproteins. The lipoproteins transport lipids and some of these are familiar, e.g., LDL (low density lipoprotein), HDL. Triglycerides in the blood are carried in these particles. So this is probably the triglycerides you read about.
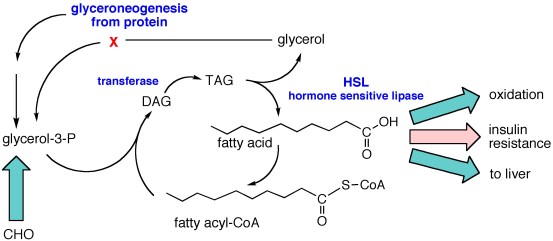
Lipoproteins are the transporters of lipids. TAG, in particular, is brought into cells by another lipase (lipoprotein lipase or LPL) on the cell surface that removes the fatty acids. In other words, to be absorbed the TAG is broken down into fatty acids again. Once absorbed, the fatty acids can be oxidized for fuel or, once again can be re-synthesized, step-wise: → MAG → diacylglycerol (DAG) → TAG. Here’s the summary figure:
Bottom line:
Fat (TAG) is continually broken down and re-synthesized. The breakdown process is called lipolysis and the lipolysis-synthesis cycle goes on in different places in the body but notably in fat cells. An interesting thing about fat cells is the way they carry out the cycle. Lipolysis is a simple process but synthesis is complicated. Speaking in energy terms, it is easy to break down nutrients. It requires energy to put them back together. To make TAG, either the glycerol or the fatty acid has to be “activated”: so the actual reactive form is a molecule called fatty acyl-coenzyme A or fatty acyl-CoA (pr. Co-A).
Glycerol-phosphate.
Biochemical reactions almost never run by themselves even if energetically favorable — you have to distinguish between whether the reaction goes forward (energy) and how fast it will go forward (rate) — but are rather controlled by catalysts, that is, enzymes. The enzyme that catalyzes the first step in the reaction, a transferase, will not work with glycerol itself. The enzyme requires a particular form of glycerol, glycerol-phosphate. The special characteristic of the fat cell is that the glycerol-phosphate that is required for re-synthesizing fat cannot be made directly from glycerol as it can, for example, in the liver which also has an active fatty acid-TAG cycle. In order to make glycerol phosphate, fat cells require glucose, or at least we thought that they did. In the absence of glucose, as in starvation or a low carbohydrate diet, fat synthesis is repressed. At the same time, the enzyme that catalyzes breakdown, hormone-sensitive lipase, is enhanced because it is turned on by glucagon and turned off by insulin. These are the hormones in the term “hormone-sensitive lipase” (HSL).
This was the original rationalization for the apparent advantage in a low-carbohydrate diet: without carbohydrate, the adipocyte would not be able to supply glycerol-phosphate and the fatty acid-TAG cycle would go largely in one direction: breakdown to produce fatty acids and this is undoubtedly one of the major effects.
It turns out, however, that the fat cells protect stores of energy in fat by other methods. We now understand that cells run a process called glyceroneogenesis which is a truncated form of gluconeogenesis and it supplies an intermediate in the synthesis of glucose and this can be converted to glycerol-phosphate. Generally, especially if the diet is hypocaloric, the net effect is to break down fat and supply fatty acids as a fuel for other cells. Fatty acids circulate in the blood bound to a protein called albumin. Under conditions where there is higher carbohydrate, however, and the fatty acids are not being used for fuel, they can stimulate insulin resistance. So, fatty acids in the blood are a good thing if you are breaking down fat to supply energy. They are not so good if you are over-consuming energy or carbohydrates because, in the presence of insulin, they can lead to insulin resistance.
Summary:
Triglycerides are made of three fatty acids. There is a continual fatty acid-TAG cycle that goes on all the time in different cells. The resynthesis of fat in the adipocyte requires glycerol-phosphate which can come from carbohydrate metabolism or from glyceroneogenesis, the truncated form of gluconeogenesis. Triglycerides in the blood are carried in lipoprotein particles, chylomicrons, LDL, HDL. Fatty acids in the blood are carried by the protein albumin.

Very useful update but would love more details on glycerogenesis.
For future posts. We also lost from comments from trying to separate this from main posts. Will try to fix that too.
I, too, appreciated this update. I also appreciated the videos referenced in the original post. You have slightly demystified organic chemistry for me. Thanks.
Thanks.
I understand that once the fatty acids are released from the fast tissue via lipolysis, they are either recycled back into fat cells or oxidized via beta-oxidation. If one is low carb with medium protein, but not able to oxidize fat, does this signal insulin resistance? What more can one do to energize beta-oxidation in the mitochondria?
Apologies for delay in answering but I am not sure that there is simple answer at the whole body level. What makes you think that you are not able to oxidize fat? I don’t think we have such fine-tuned access to our mitochondria.
Very informative. I really appreciate this post. So much things I learned and I have so much to learn from your post. Anticipating to your next update. The basic knowledge that I have known about fatty acids, it is essential in our body health because we can’t synthesize it on our own, instead it should be ingested through diet. My main source to synthesizing fatty acid is including salmon in my diet almost everyday because it is rich in omega-3 and a study has shown that intake of long chain omega-3 increase to achieve better health. According to Dr. Oz on his show that a coleus plant or also known as forskolin can release fatty acids from adipose tissue, and associated with carbohydrates and fats are required to produce enough metabolic energy and increase thermogenesis resulting in the loss of body fat.